Risk Groups and Factors
WHO IS AT GREATER RISK?
Respiratory Syncytial Virus (RSV): is a common cause of respiratory infection in infants and children that can result in respiratory infection in infants and children that can result in bronchiolitis or pneumonia.1
Higher-Risk Populations Include Preterm Infants and Children <2 Years Old With BPD or HSCHD2,3
It is estimated that
15M
babies are born preterm (before 37 completed weeks of gestation)4
1st
BPD is most common sequela of preterm birth5
Infants with
CHD
have been shown to be at increased risk of RSV-related morbidity and a higher mortality rate compared with children without cardiac disease3
Other high-risk groups* vulnerable to RSV are children with neuromuscular impairment, immunodeficiency, and Down’s syndrome3
*SYNAGIS® is not indicated in these other high risk groups across all countries.
PREMATURE BIRTH
Worldwide, approximately 1 in 10 babies are born premature6.
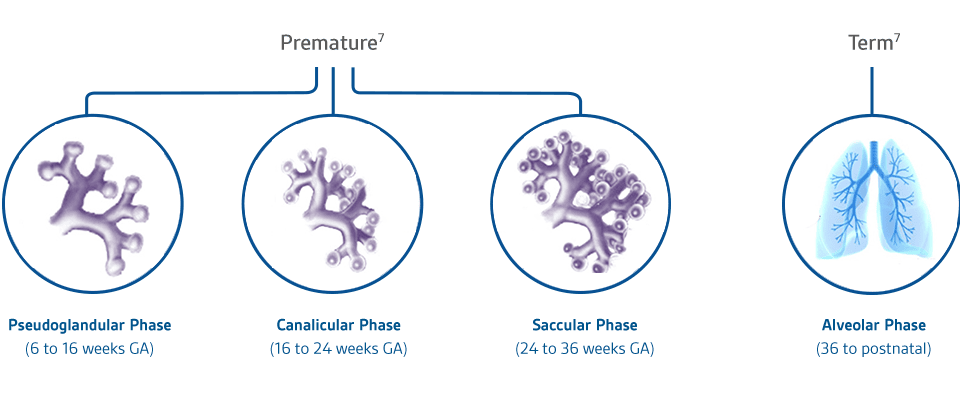
Premature7
Pseudoglandular
(6 to 16 weeks GA)
Canalicular Phase
(16 to 24 weeks GA)
Saccular Phase
(24 to 36 weeks GA)
Term7
Alveolar Phase
(36 to postnatal)
Although alveoli are present in some infant's lungs as early as 30 to 32 wGA, they are not uniformly present until 36 weeks GA.7
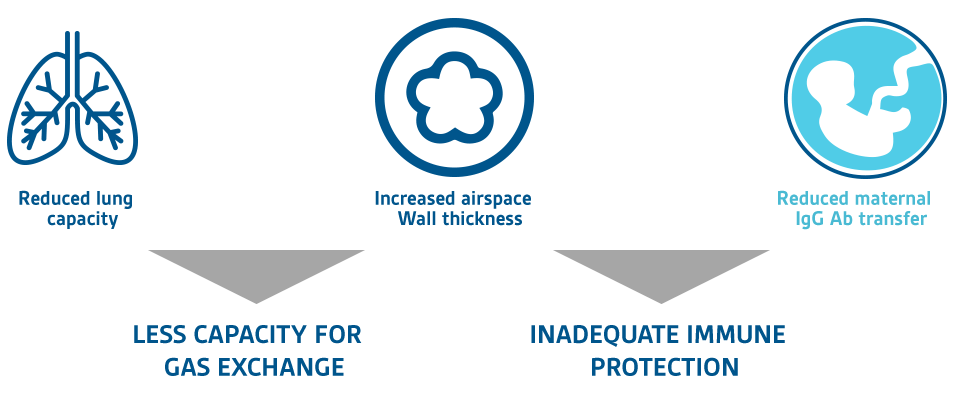
PRETERM INFANTS ARE AT HIGHER RISK FOR SEVERE RESPIRATORY INFECTIONS
Risk factors for severe RSV illness in premature infants relative to full‐term infants8
Premature infants (34-36 wGA) have a normal physical appearance, but they may have under developed lungs at birth, persistently reduced airway function throughout the first years of life7
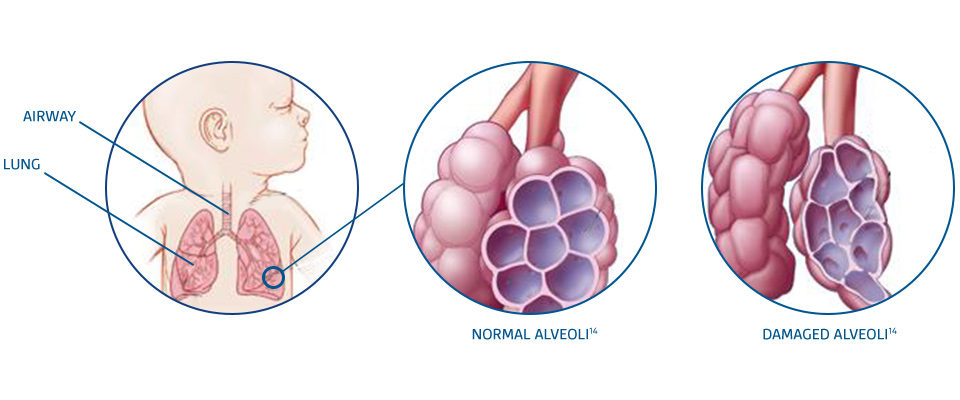
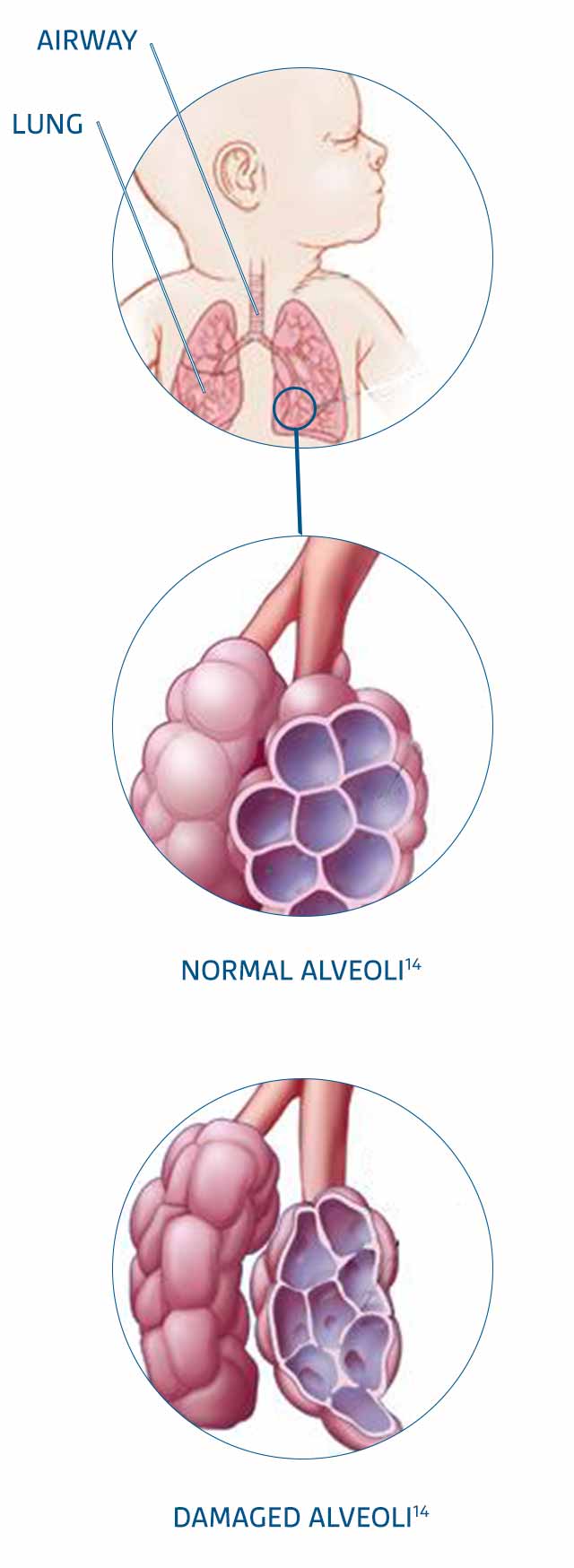
BRONCHOPULMONARY DYSPLASIA
Premature infants with BPD are at increased risk of serious RSV-induced LRTIs and rehospitalisation3,9
BPD is the most common medical complication associated with extreme prematurity (less than 28 wGA)10
Underfunctioning airways and underdeveloped, damaged alveoli can increase the need for ventilation support after a serious acute LRTI3,11-13
BPD amplifies the risk of severe infections by2:
- Limiting pulmonary functional reserve
- Distorting airway architecture
- Promoting a proinflammatory milieu
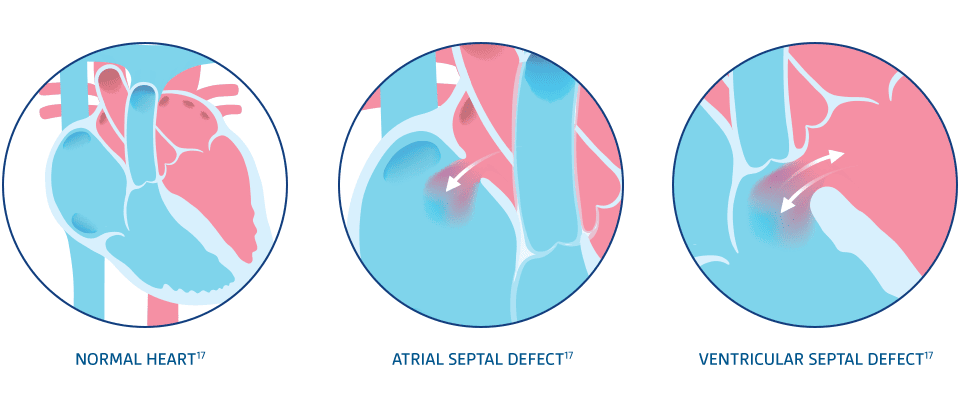
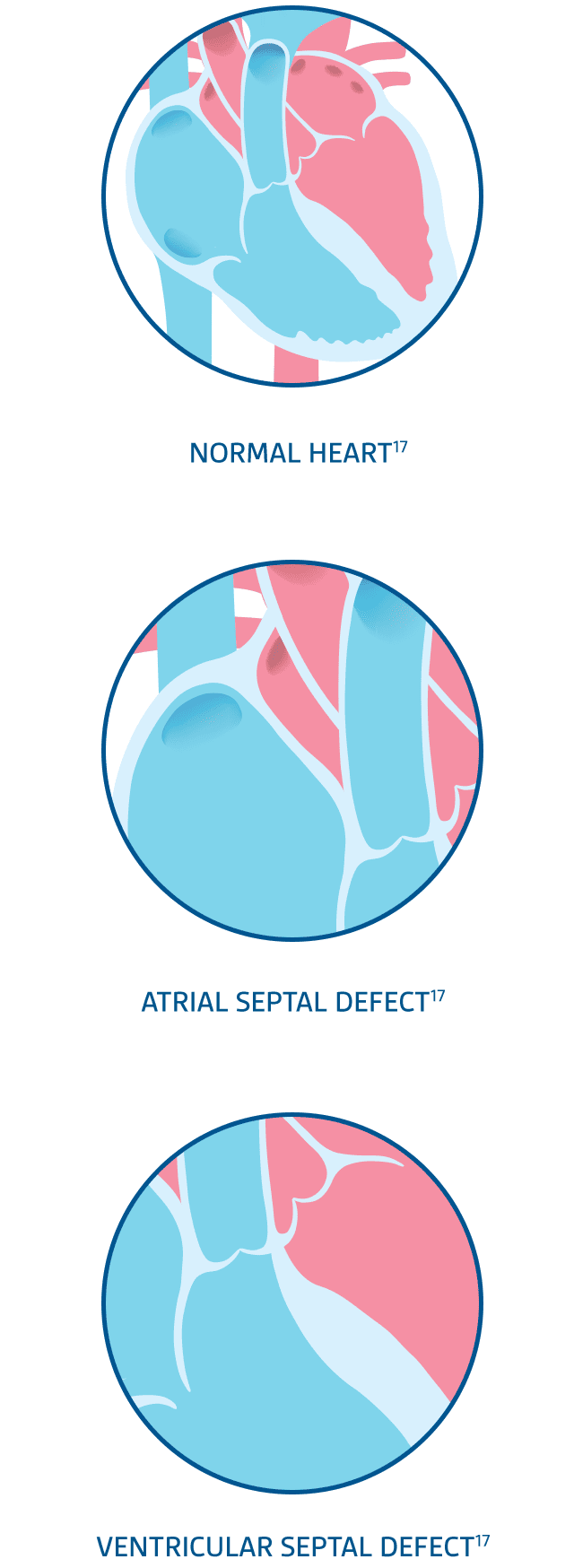
CONGENITAL HEART DISEASE
CHD increases the risk of respiratory or cardiac failure with RSV-related LRTIs3,15
CHD is the most commonly diagnosed congenital disorder in newborns, afflicting approximately 0.8% to 1.2% of live births worldwide16
CHD often involves clinical complications following an RSV infection3,15
- Limited ability to increase cardiac output and oxygen delivery
- Increased need for assisted ventilation or longer duration of oxygen supplementation
Infants and young children with cardiac disorders due to CHD have increased susceptibility to RSV infection.18
OTHER RISK FACTORS
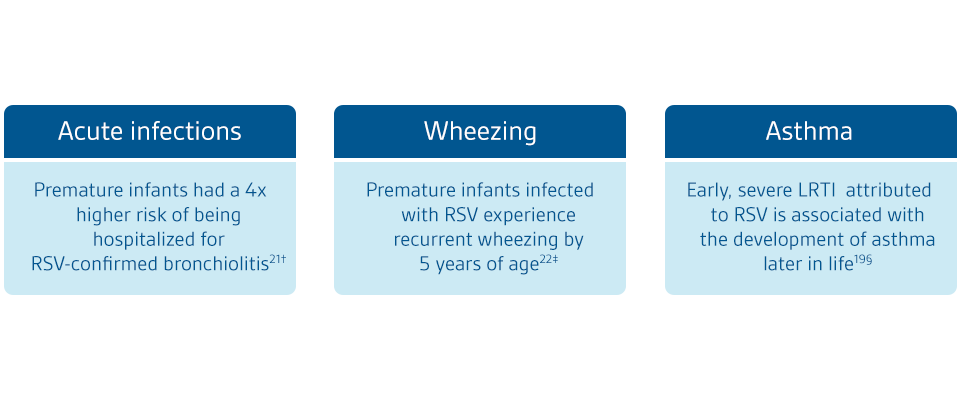
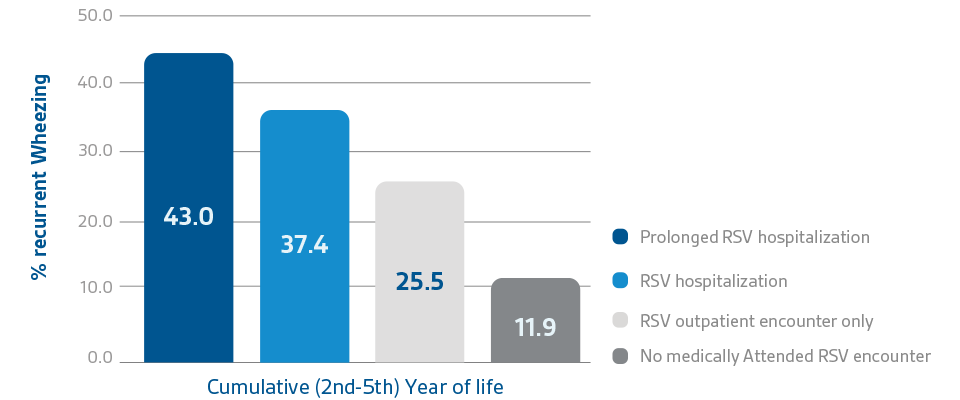
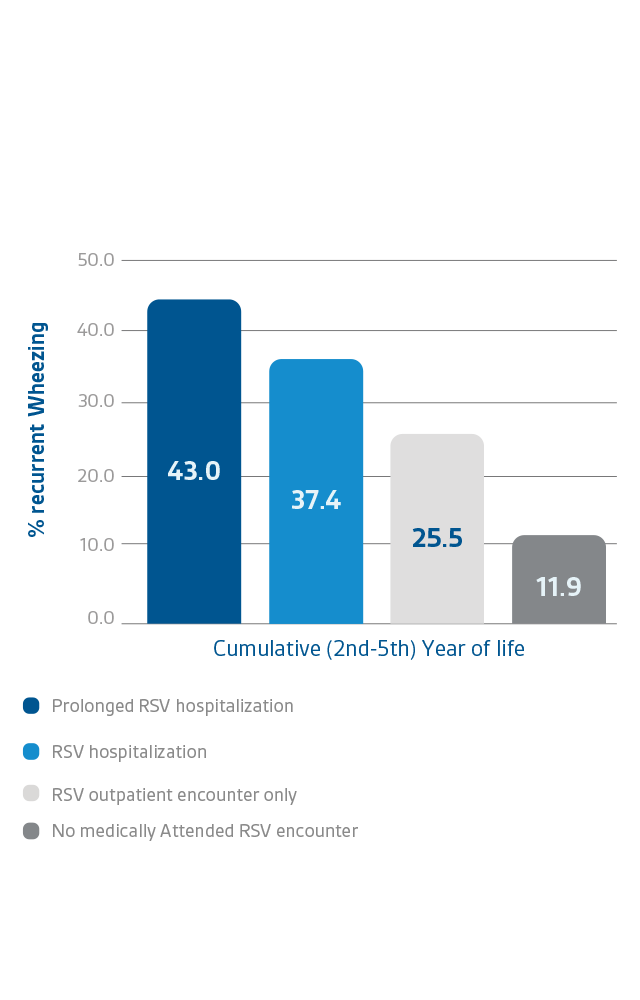
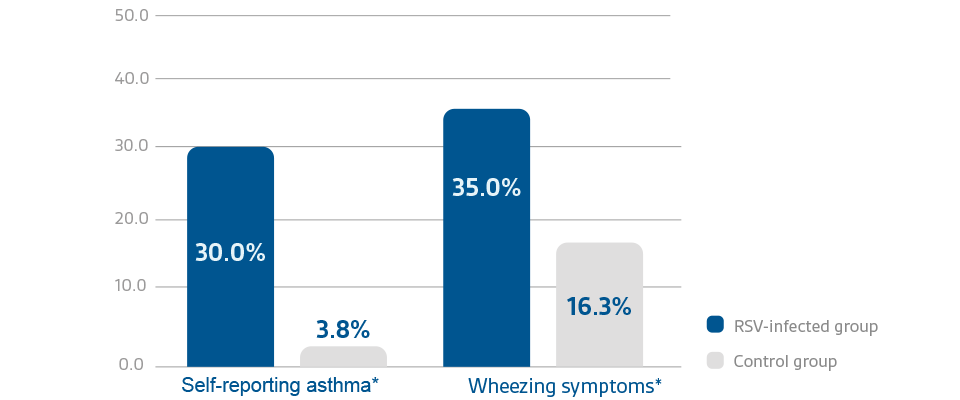
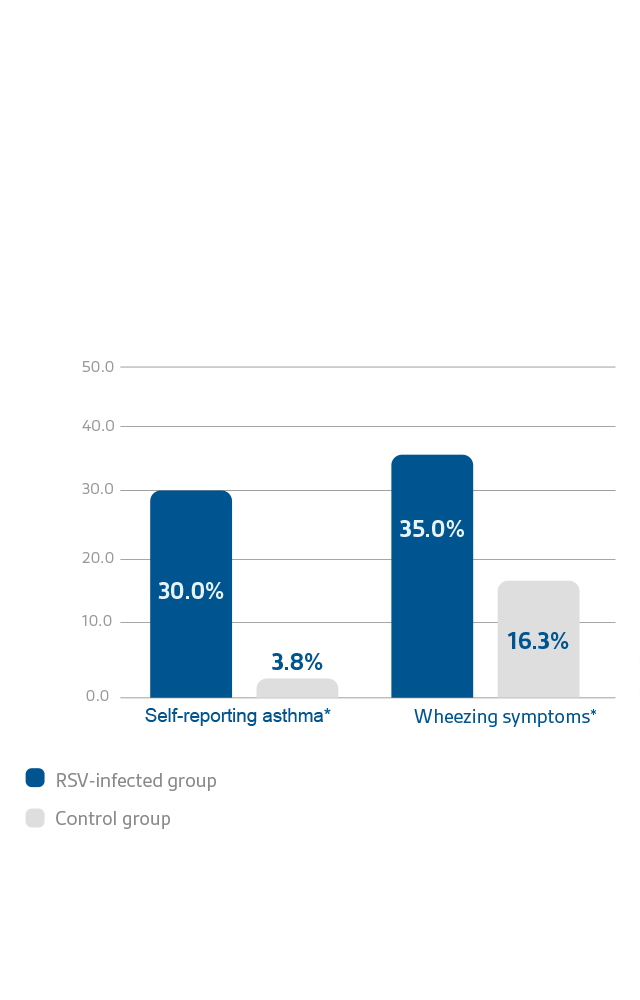
Morbidity (wheezing / asthma)
RSV infections can lead to severe disease in high-risk groups with short and long-term consequences19,20
*This is a survey-based study conducted among adults (median age: 27 years) who were hospitalized for RSV-associated viral bronchiolitis and/or pneumonia at infancy (during 1981-1982) and followed up for >25 years. A questionnaire was sent in 2008 to the subjects with early RSV hospitalisation. It evaluated the outcomes such as self-reported asthma and wheezing symptoms in this patient population hospitalised for RSV infection at <24 months of age.
†The goal of this study was to compare hospitalisation rates for bronchiolitis (RSV-confirmed and all types) between very preterm infants (33 weeks' gestational age, wGA) without bronchopulmonary dysplasia and full-term infants (39–41 wGA) during the 2008–2009 respiratory syncytial virus (RSV) season in France. Infants were eligible if they were under the age of six months at the start of the RSV season in 2008–2009. The primary outcome was to compare RSV-confirmed bronchiolitis hospitalisation rates between a group of preterm infants 33 wGA without BPD and a group of matched full-term newborns followed up over the 2008–2009 RSV season in France.
‡Between 1996 and 2004, a retrospective cohort research looked at children born at 32 weeks gestation. Recurrent wheeze in the fifth year of life was the primary endpoint, and it was linked to laboratory-confirmed, medically-attended RSV infection in the first year, prematurity, and supplemental oxygen during newborn hospitalisation.
§A comprehensive review of publications published between January 1, 1995, and December 31, 2015 was conducted. The researchers included studies that looked at the incidence and long-term effects of RSV LRTI in children. The goal of this fifth article was to find out how long RSV lower respiratory tract infection (RSV LRTI) in early infancy causes long-term respiratory morbidity.
Find out whether your patient is at high risk for serious RSV disease and may benefit from prophylaxis with SYNAGIS.
For full safety and prescribing information, please see the SYNAGIS Summary of Product Characteristics (SmPC).
Ab = antibody; BPD = bronchopulmonary dysplasia/disorder; CHD = congenital heart disease; GA = gestational age; HSCHD = haemodynamically significant congenital heart disease; ICU = intensive care unit; IgG = immunoglobulin G; LRTI = lower respiratory tract infection; RSV = respiratory syncytial virus; wGA = weeks gestational age
References: 1. Tsolia, M, et al. Eur J Epidemiol. 2003; 18, 55–61. 2. Piedimonte G, et al. Pediatr Rev. 2014;35(12):519-530. 3. Sommer C, et al. Open Microbiol J. 2011;5:144-154. 4.World Health Organization. Preterm birth. Published February 19, 2018. https://www.who.int/news-room/fact-sheets/detail/preterm-birth Accessed February 2022. 5.Jensen EA, et al. Clinical and Molecular Teratology. 2014; 100:145-157. 6. Hannah Blencowe. Reproductive Health. 2013;(10):Suppl 1,S2. 7. Andrew A, et al. Pediatrics. 2010;126(1):115-128. 8. Speer ME, Good AB. Clin Med Ther 2009:1:459–469. 9. Chaw SP et al. J Infect Dis 2020; 222(suppl 7): S620-S627. 10. Thébaud B et al. Nat Rev Dis Primers 2019; 5(1): 78. 11. Hussain M et al. Biochem Biophys Acta Mol Basis Dis. 2017; 1863(12): 3226-3242. 12. Greenspan JS. Bronchopulmonary dysplasia (BPD). Kids Health from Nemours. https://kidshealth.org/en/parents/bpd.html. Accessed February. 13. Bhandari A et al. Front Biosci 2003; 8: e370-e380. 14. Bronchopulmonary Dysplasia (BPD) in the Premature Infant. Saint Luke’s Health System. https://www.saintlukeskc.org/health-library/bronchopulmonary-dysplasia-bpd-premature-infant. Accessed September 2021. 15. Canadian Paediatric Society. Paediatr Child Health. 2003;8(10):631-633. 16. Wu W, et al. Medicine (Baltimore). 2020;99(23):e20593. 17. Atrial and Ventricular Septal Defects - Children’s Health Issues. Merck Manuals Consumer Version. https://www.merckmanuals.com/home/children-s-health-issues/ birth-defects-of-the-heart/atrial-and-ventricular-septal-defects#. Accessed February 2022. 18. Calbaka AK. Pediatr infect Dis.J2004:23: S41-S45. 19. Brigitte F, et al. Infect Dis Ther. (2017) 6:173–197. 20. Palmer L, et al. Curr Med Res Opin. 2011;27:403–412. 21. Gouyon JB, Rozé JC, Guillermet-Fromentin C, et al. Epidemiol Infect. 2013;141:816–826. [PMC free article] [PubMed]. 22. Escobar, et al. BMC Pediatrics. 2013 13:97. 23. Ruotsalainen M, et al. Pediatr Infect Dis J. 2010;29(9):872-4.

.png)